 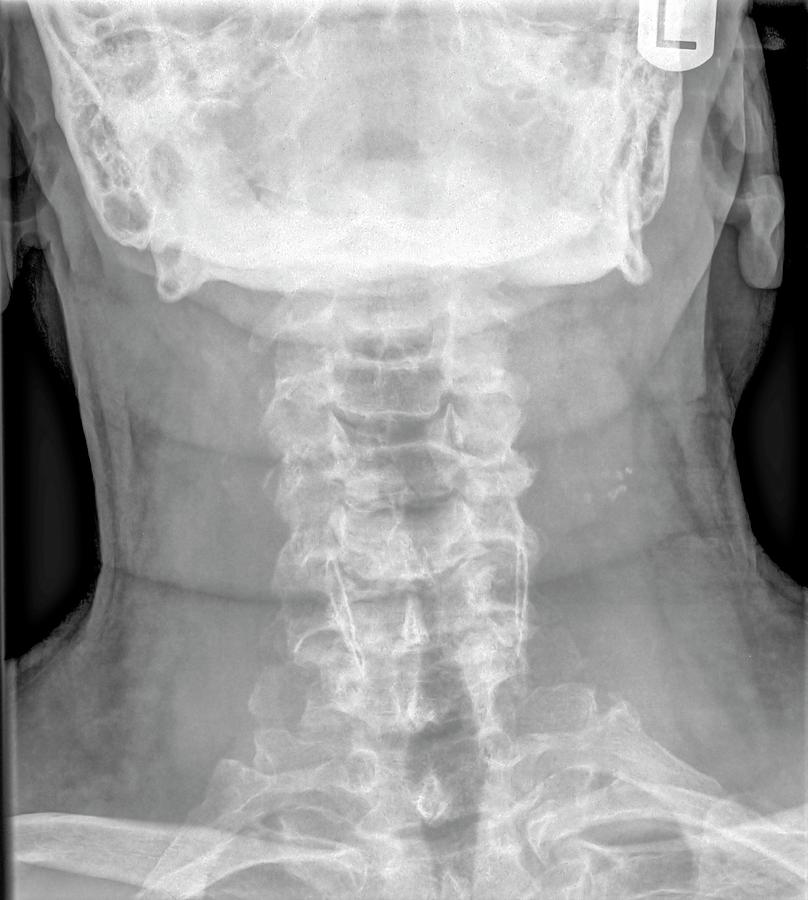
The patient was ambulatory with a walking stick at 6 months post-operativelyĬervical spine was immobilized postoperatively for 12 weeks in a halo fixation deviceįollow-up plain radiographs and a thin cut CT demonstrated stable positioning of the instrumentation and a solid sheet of bone from the left atlantooccipital and atlantoaxial joints on the left extending to C–4. 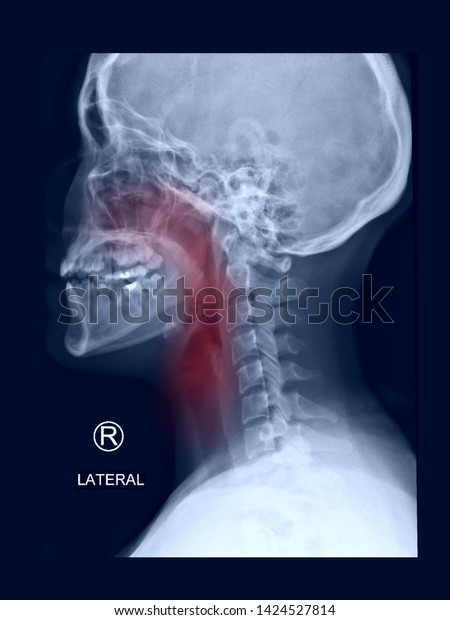
X-rays performed at 12 weeks showed stability of the C1–C2 complex after the halo was removal. Second case: underwent also two stages, 1st was anterior approach for dens resection then posterior approach for fusion and stabilizationįirst case the plan initially was emergent anterior approach (C2 hemilaminectomy) but the expert surgeon was not available, so case was managed all dorsally then patient was observed for 12 days on antibiotics and still patient is symptomatic, and MRI showed no improvement.īoth patients were followed up to three years with good outcomes, MRI was the modality for follow upįirst case: the decision was made to perform anterior approach after they noticed the patient did not improve clinically and radiologically Second case: the patient underwent two stages, anteriorly for dens resection and after 14 days with antibiotics and immobilization with Halo fixator placement, patient was taken to second stage which is posterior fusion and stabilization. Additionally, we emphasize the importance of stabilization to successfully treat spine osteomyelitis and summarize the literature available discussing upper cervical spine infection treatment options.Ĭomplete re-ossification & fusion on follow up CTĪnterior approach was an option but due to patient condition and comorbidities, patient was managed all from posteriorįirst case: underwent two stages, 1st was posterior approach and the 2nd was anterior approach 
We hereby describe the case of a middle-aged gentleman who presented with a pyogenic infection involving the occipital condyles, the atlas and the axis with severe instability to show that the posterior approach without the anterior transoral approach is a valid surgical option in these cases. We found only 15 papers about upper cervical osteomyelitis in English literature from 1995 to 2020. The reason behind this is due to its unusual location and relatively rare occurrence. The delay in diagnosing upper cervical osteomyelitis might result in undesirable management delays, which could lead to instability and neurological deficits. High clinical suspicion is needed to reach the diagnosis. Besides, upper cervical pyogenic infection diagnosis can be challenging patients usually present with vague symptoms, and the occiptocervical pain may not be severe. Several factors have been recognized in the literature, potentially predisposing to the development of C1-C2 osteomyelitis, including the elderly population, immunocompromised patients, and patients with associated comorbidities, such as diabetes, hypertension, and end-stage renal disease. Upper cervical spine pyogenic infection is not common compared to other vertebral segment infections, and it is usually associated with unfavorable clinical outcomes. Among these, only 3%–12% are confined to the cervical spine. Pyogenic infections of the spine are generally rare, representing about 3%–4% of all bone infections. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
